March 30, 2012
confusion
It's confusing, all this. It's hard to know just exactly who is walking through the doors of the medical center sometimes. I was here a time or three with my brother. And then my dad. Sometimes at the same time. My brother died. My dad did well. So a break. Then I came here a physician in training. Saw patients who resembled both my dad and my brother.
Now it's spring break and I'm spending it here again. My dad's stem cell transplant. It's hard to know what emotion, what thought, what gut feeling goes with which experience. It's like an alcoholic training to be a bartender. It's like having to work at a cemetery where your loved ones are buried. You have to keep going back and face physical manifestations of your pain. Every day. Study the diseases that can wreak havoc. That can kill. Except it's not only a cemetery. It's the site of my dad's hope. It's where I am being trained in my profession. Evolution of a complex love-hate relationship. Confusing.
March 29, 2012
relative
So all things considered, yeah, it couldn't have gone any smoother for my dad. Infections, drug reactions, arrhythmia, mild graft-versus-host. Those were all just minor hiccups relatively speaking. We're just three weeks after the stem cell transplant and he's been given permission to go home for the weekend. That pretty much says it all.
March 28, 2012
March 20, 2012
discharge
Now the leash has been let out a bit. It's still there. It's just long enough to extend out of the hospital, but not so long as to allow my dad to go back home. They have to live within 15-20 minutes distance of the hospital in case of a fever or some such crisis. He will have to come back daily to MDACC for 2 straight weeks. His blood will be checked and various treatments will be administered. But no more being hooked up to an infusion pump 24/7. He can go into a bedroom, albeit a new and strange one at an apartment, and go to sleep uninterrupted.
This is a huge milestone to reach and with each point, the imminent risk decreases a bit. The first 10 days was the most crucial and dangerous. By day 10, engraftment usually begins and the counts start to come back up. He made that one quite nicely, despite all the side ventures. The next major hurdle is being well enough to be discharged. He's crossing that threshold now. To make it to 100 days post transplant is the next goal to set his focus upon. Somewhere around that time, if all goes well, the leash gets a lot longer and the patient is allowed to go back home. My dad is on day 20 so only approximately 80 more days to go.
March 18, 2012
update
But then a rash appeared. No pain or itching, fortunately. Interestingly, it first appeared where his skin had already been agitated by the EKG electrodes. It then spread around to his neck and back. Both the urine and blood cultures came back negative for any bacteria. That doesn't mean it's not an infection. Maybe, maybe not. If it is, you don't know which bug(s) you are facing. Couple that with the rash and it shifted the possibility of infection towards drug reaction. Maybe, maybe not. When he started getting the urinary symptoms again on Thursday, they changed antibiotics to meropenem, which is a relative of penicillin. Any of the the penicillin type drugs can cause allergic reactions. So they stopped that drug. They switched to cipro in case it is an infectious process. And more steroids. Can't forget those. That quickly brought the fever under control.
And on they charged with the last (hopefully) round of chemotherapy on the schedule. SCT transplant is a bit like surgery in that regards. Once the patient is cut open, you can't stop. You react and deal with each crisis as it comes. You can't just wait and see how the patient feels. So it goes with SCT. The cells have been injected. The chemotherapies must continue despite the fever. More steroids and rituximab and that was uneventful. Saturday came and went and my dad actually felt good. Good enough to actually eat. Good enough to actually be able to watch TV. Yes, even watching TV is a chore during this process. It's probably a good benchmark to know how difficult something is if watching TV becomes too onerous and difficult. His blood counts continued to look good which meant the engraftment was likely happening. Usually it's around day 10. Saturday was day 9. Sunday was day 10. There was talk of an early discharge if this kept up.
But on Sunday, my dad spiked another fever back up to 103. More steroids and tylenol. Rash, too. Only this one hurts. And again, it gets nebulous. Is it infection? Is it drug reaction? Is it graft-versus-host? All of the above to some extent? We'll probably never know definitively. That's the art of medicine. You treat empirically on your best guess based on experience and hunches about the patient. Reassess and readjust the gameplan accordingly. One thing is certain, though. Any talk of him being discharged tomorrow is certainly out of the question.
March 15, 2012
March 14, 2012
keepin' movin'
But I've never gone through chemo, much less chemo and a stem cell transplant and the endless therapies which accompany it. From watching my dad, near as I can imagine is that it's like having mono, the flu and a hangover all at the same time. Everything aches. The mere thought of food is repulsive. And you just want to sleep all the time but they won't let you. And that makes my dad's door all the more impressive. Who in the world would want to exercise with all that going on? He traded in some of his M&Ms for a banner. Each banner is worth 15 M&Ms so by my count, he racked up 44 exercising bouts in 12 days - a bit over the requisite 3 per day. Good job!
March 13, 2012
Tally
1) A fever due to a UTI which was treated which with two antibiotics. They worked. He's still on them.
2) Two superficial clots - one in his arm and one in his leg. They are being treated with a type of heparin (an anticoagulant) called lovenox to make sure he doesn't get the dangerous deep ones. He's still on it which is good - see below.
3) A bout of arrhythmia which was an averted disaster due to digoxin. One of the big dangers with a-fib is throwing a clot and causing a stroke. Since he was already on lovenox, he got a two-for-one benefit there. He's out of the woods but this will be a difficult one to manage going forward.
Despite a crisis every other day, he's still doing better than some of the patients I see on the floor. It's a rough business, this one.
Isaac
Sent from my iPhone
new addition
Well, we now know that dose is not sufficient to control his arrhythmia. It came back with a vengeance last night. On a scale of 1-10 for the severity of crisis (10 being oh shit!), it was about a 4. They gave more metoprolol but it didnt respond. Give more? Can't. His bp was getting uncomfortably low. Crisis number starting to creep up. Digitalis time? Wait, his serum potassium levels were already out of whack. Corrected that and they had to give digoxin to cardiovert his heart back into normal rhythm. He was close to being transferred to the ICU (intensive care unit) but fortunately the digitalis worked. It was a rough night for him, which is an understatement.
Now the challenge moving forward will be finding that sweet spot of a metoprolol dose which controls the arrhythmia but allows him sufficient blood pressure and heart rate that is compatible with remaining upright and coherent. His heart rate was running in the 50s today and that was after his exercise. He's continuing to walk that razor's edge and conquer each crisis.
March 11, 2012
new job
March 10, 2012
update
But there are always lingering challenges. Accompanying the UTI, but not necessarily caused by it, my dad gained 11 pounds, 7 of which was in less than 30 hours. Originally, my dad was proud that his weight was holding steady, despite not eating. That obviously violates the laws of thermodynamics. The weight had to be water weight but you still hold onto what you can. When he started gaining weight, he accepted that it was water. He gained more. His intake was much greater than his output. Simple math but it can lead to complications with the kidneys and/or bladder. So they put him on lasix to pull the water and salt off him. And it worked. He started trips to the bathroom every 15 minutes. Good thing, too, because if Vitamin L doesn't work, it's a foley catheter and those are, shall we say less than pleasant.
Exhausted and drained, my dad feels "better" today, at least with respect to the lack of a UTI. Fatigue is increasing daily, if not hourly, as his blood counts begin to plummet. Less red blood cells mean less ability to carry oxygen. Anyone who's suffered severe anemia can attest to the fatigue. So he continues to walk and sleep and urinate, walk and sleep and urinate. "When the hell did I enter a nursing home?" he laughed.
The first 10 days after the SCT transplant are crucial. It's also when the patient feels the worst and unfortunately, when the exercise and eating matters the most. Of course, exercise and eating are the last things they want to do so I'm sure he'd appreciate hearing some encouragement via his blog or email.
what's a stem cell transplant look like
The process leading up to the transplant varies according to the patient, the type of cancer and the type of transplant they receive. It involves admission to the hospital for 1-2 weeks prior to the transplant where they will receive the chemo appropriate to them. Gone are the days where they irradiate the person to knock out the bone marrow. You can get much better success with lower doses of chemo.
While the patient is doing their thing, a whole other process is being coordinated. It's like cooking multiple dishes and having them all finish at exactly the same time. Behind the scenes that we don't see is the stem cell collection. We don't see it because my dad's was an unrelated donor. All that we know is that he is a he and 37 years old. He either gave the cells at an institution near his home or he was actually flown in to MD Anderson. He would've gone through a battery of tests to insure he was in good health similar to the ones my uncle went through. They were fresh stem cells, not frozen, and they were collected at about 2 pm the day before. If out of town, they would've been flown in, probably by a medical courier like organ transplants. The lab would've then cleaned them up and resuspended them in some new media.
Because all that collection is happening somewhere else, we didn't actually know the time of the transplant. We found out the morning of the transplant. Originally it was scheduled at 1:15 pm which then was bumped up to 11:30 am. I can't remember MDACC ever being ahead of schedule on something. I think this was a first but what a day to be early.
The morning of the transplant the doctor walks in with his entourage of fellow, nurse, PA, and pharmacist. He exams my dad briefly and assures us that everything is a green light. My dad was given the premedications of steroids and benadryl to prevent any reaction. At about 11:00 am, the nurse walked in with the cells while also teaching a nursing student (they have to learn on somebody, right?). And here they are. Only 284 milliliters. A little more than a cup. But, oh, but what's in that cup....big things in small packages and all that.
My dad understandably wished to hold them. He held them high, asked for the Lord's blessing and graciously thanked whomever donated them.
The doc peaked his head in the door and gave his thumbs up. The chaplain read a bible verse while the nurse began attaching the cells to his IV line. The nurse remained in the room the entire time to make sure it goes off without a hitch. The bag emptied by simple gravity and was done in less than 45 minutes.
March 9, 2012
Promotion
humor as your weapon
though the weather be foul
On you will go
though your enemies prowl
On you will go
though the Hakken-Kraks howl
Onward up many
a frightening creek,
though your arms may get sore
and your sneakers may leak.
On and on you will hike
and I know you'll hike far
and face up to your problems
whatever they are.
You'll get mixed up, of course,
as you already know.
You'll get mixed up
with many strange birds as you go.
So be sure when you step.
Step with care and great tact
and remember that Life's
a Great Balancing Act.
Just never forget to be dexterous and deft.
And never mix up your right foot with your left.
March 8, 2012
happy birthday!
"I've got new homes for all 4 million of you," my dad says to his own body while pointing to his bones.
As tears started to come to my eyes, I was overwhelmed by how arduous the journey has been. When life has whipped you so many times, it's all too easy to lose track of just how far you've come. So many times the fate of this journey could have changed on the smallest of fortunes. Infections, anemic crises, infections, bleeds, infections, clots, infections. And I was keenly aware of how we were missing one person in that room. How my brother would've loved to see this for our dad. It's so very confusing feeling elation, gratitude, weariness, pride and profound loss all in the matter of a moment. The infusion finished without any bumps or problems.
With any infusion of biological products comes benadryl. With benadryl comes drowsiness. My wife and I stepped out for a bit as my dad drifted off for a well deserved rest. There on the top shelf of the gift store sat a rather goofy birthday hat which my wife spied. No, it was not my dad's birthday, at least in the conventional sense. However, the nurses on the floor view the transplant as a new birthday and cheerfully wish the patient "happy birthday" on the day of the stem cell transplant. The more we thought about it, the more we liked it so she purchased the hat and took it back to his room. We put it on him, sang "Happy Birthday" to him, and then paraded him around the entire ward. Without fail, every patient and staff member cracked a smile when they saw him and wished him "Happy Birthday". It was one of the most irreverantly touching moments I've ever had the pleasure of experiencing. Happy Birthday, Dad!
March 7, 2012
just can't eat
You'll pass the whole gang and you'll soon take the lead.
Wherever you fly, you'll be best of the best.
Wherever you go, you will top all the rest.
Except when you don't.
Because, sometimes, you won't.
I'm sorry to say so
but, sadly, it's true
that Bang-ups
and Hang-ups
can happen to you.
You can get all hung up
in a prickle-ly perch.
And your gang will fly on.
You'll be left in a Lurch.
You'll come down from the Lurch
with an unpleasant bump.
And the chances are, then,
that you'll be in a Slump.
And when you're in a Slump,
you're not in for much fun.
Un-slumping yourself
is not easily done.
growing M&M's
NO!
That's not for you!
Somehow you'll escape
all that waiting and staying
You'll find the bright places
where Boom Bands are playing.
With banner flip-flapping,
once more you'll ride high!
Ready for anything under the sky.
Ready because you're that kind of a guy!
March 6, 2012
platitudes & choices
March 5, 2012
Waiting
that you'll start in to race
down long wiggled roads at a break-necking pace
and grind on for miles across weirdish wild space,
headed, I fear, toward a most useless place.
The Waiting Place...
...for people just waiting.
Waiting for a train to go
or a bus to come, or a plane to go
or the mail to come, or the rain to go
or the phone to ring, or the snow to snow
or waiting around for a Yes or a No
or waiting for their hair to grow.
Everyone is just waiting.
Waiting for the fish to bite
or waiting for wind to fly a kite
or waiting around for Friday night
or waiting, perhaps, for their Uncle Jake
or a pot to boil, or a Better Break
or a string of pearls, or a pair of pants
or a wig with curls, or Another Chance.
Everyone is just waiting.
March 4, 2012
M&M
"They have these little construction paper circles called M&M. It stands for "moving" and "motivation". When you leave your room to exercise, you punch it into a time stamp kinda like a factory worker. You then clock back in and tape the construction paper to your room door. Once you earn enough, you trade the circles in for a banner. It's a way of showing the doc how much you've been exercising because they want you moving as much as possible. Here's your papa's door after the first day."
My son, ever the teenager smart ass chuckles and replies, "Sounds like kindergarten."
"Yeah, it does. But when you're fighting for your life, you do what you gotta do."
My dad said it feels like he's in kindergarten, too. But everytime we leave the room, he makes sure we grab one of those M&Ms to tape to the door. My dad is more resolved, more resolute, more determined than I've seen him in a long, long time. All the fear, apprehension and uncertainties are still there. But beneath it all is still a determination and will that is growing. It's a joy to see.
March 3, 2012
Out of prison
I have beautifully bitter sweet memories of eating my dinners while my brother had late nights of chemo. The smell of food made him nauseous so I'd go outside into the gardens of mdacc for a brief respite.
the view from here
Yesterday, while my dad received Day -6 Treatment, our conversation stumbled back to that gentleman who went quietly into that dark night. "I won't even be able to go out in the sun anymore," and to anyone who knows my dad who made his living by the sweat of his brow, that's no small thing. A decent sun exposure could trigger a graft-versus-host reaction even years afterwards. The price of cancer.
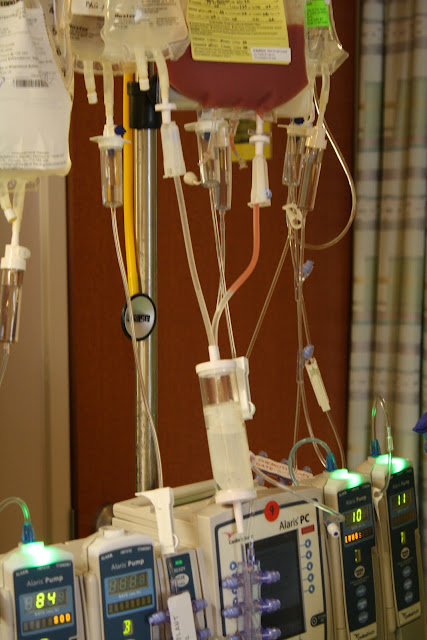
The view of life changes in ways unimagineable, both literally and philosophically. Physically, here's the view from my dad's vantage point. For the next month, I'm not sure there will ever be a point that this pole with its various bags hanging will not be hooked up to him. It's become an extension of his body. He can't go to the bathroom without it.
And here's the view from his room. Ah, what beauty is the concrete jungle of a major med center. My dad can't go outside for the next month either. So the view through the windows will have to suffice.
When faced with the daunting struggle ahead of him, I think for the briefest of moments, he might have empathized with the gentleman who said, "I'm done." After all, even prisoners get to go outside. To which my dad responded matter-of-factly, "yeah, but this gives me a chance at life." There is definitely still fight left in him yet.
March 2, 2012
fuzzy little test tubes
It's not talked about much but the way society produces the next generation of doctors is by allowing them to practice and learn on humans. It's the only way. Everybody wants new doctors but nobody wants to be the one that the resident or medical student learns on. Because learning means mistakes. Some go unnoticed, some are minor inconveniences, some just piss off the patient, but there is the very real chance for dangerous ones, too.
In my years working as a research scientist, I experimented on animals. And I mean a LOT of animals. Mostly mice, but there were rats, guinea pigs, hamsters, rabbits, and dogs thrown in, too. I had no problem rationalizing it. I looked at them as "fuzzy little test tubes." And in that time, I probably did thousands of surgeries. If I had a "bad day" doing surgery, I could always get another mouse. They breed like rabbits after all.
But now that I'm practicing and learning on humans, that's a whole different game. "Bad days" take on a whole different meaning when it's a human being's life in your hands. Intellectually, I know that I won't be perfect, that I'll miss diagnoses, that I'll make the wrong treatment plan. That's easy to say now but I know when it happens, and it will happen, it'll be a very bitter pill for me to swallow. These are not "fuzzy little test tubes." There is obviously a down side to that. But there's also an upside, which is part of the draw of medicine to me. Because they are not "fuzzy little test tubes", there is the chance for a deep and profound connection between patient and doctor.
I had not expected to experience that until later in my career but I'm starting to catch glimpses of it now. How often does one get the opportunity to be told by a dying patient, "I am not afraid of death. I have no regrets. And if I can help someone become a doctor, that's my way of giving back." There is a depth to that connection that's just not going to come up very often in the average day. But doctors seem to be offered that opportunity with at least some regularity. I'm not so naive as to think it'll happen every day, or that I won't be confronted with far too many patients whom I probably dislike vehemently on a personal level. But to at least be given that opportunity still beats working with fuzzy little test tubes.